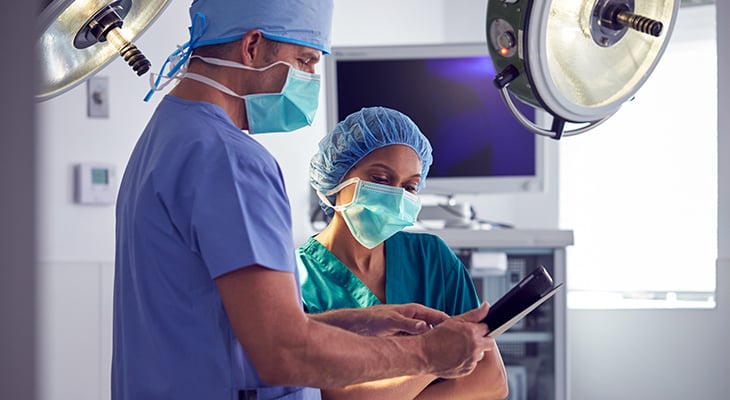
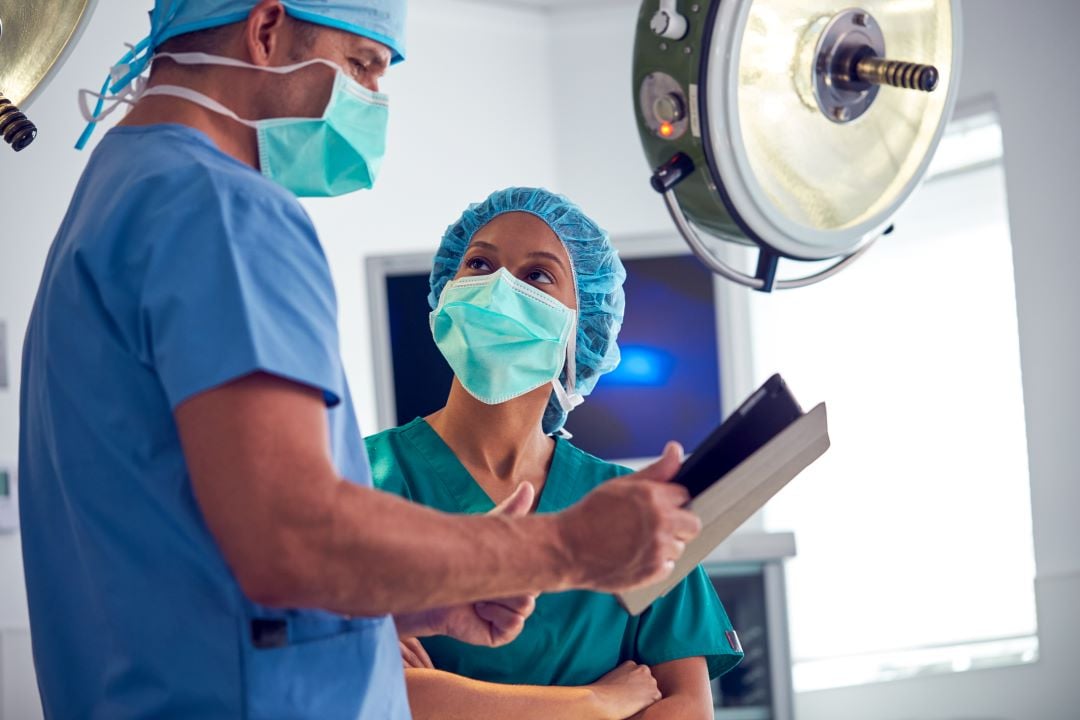
The most valuable resource in your OR is time. Efficient surgery operations rely on procedures starting on time. However, as any operating room manager knows, countless unforeseen obstacles can get in the way. For more insights on the ideal time to use surgical scheduling software, and tips to ensure the best ROI, check out this guide.
According to Becker’s Hospital Review, even slight delays due to OR turnover, or missing equipment, can impinge on efficiency and negatively impact profit margins. Furthermore, quality of care can be negatively impacted as staff scrambles to make up time. But having the right systems in place can make all the difference.
To prevent the impact of surgery delays, hospitals and ASCs are advised to take a proactive approach. A lot of emphasis is placed on the day of surgery events to minimize delays, but so much more is actually predicated on the preparation prior to the day of surgery. Understanding the most common reasons that surgeries don’t start on time and how to solve these problems is a critical first step.
Why on-time starts are vital to surgery scheduling
There are many ways in which surgery scheduling can go awry:
- Inaccuracies in surgical codes, surgery time estimates, and procedural descriptions
- Lack of preoperative preparation
- Inadequate or overcomplicated patient communication
- Outdated and inefficient data management
The cost of lost OR time runs at about $62 a minute, so wasted time is wasted money. A late first case start will have extensive impacts for the rest of the day, leading to a “cascading effect,” with progressively later starts for subsequent surgeries, and cost the OR even more if overtime is incurred. Importantly, these on-start delays can impact the quality of care your patients receive.
How to minimize delays to surgery scheduling start times
Keeping your surgery running smoothly throughout the day might seem like an impossible dream. However, with solid processes and the right surgery scheduling software, even the busiest ASC or hospital can start most surgeries on time. Follow these five steps to solve your surgery scheduling issues now:
1. Communicate clearly what is meant by “surgery start time.”
It might seem obvious, but make sure that everyone knows what is meant by “start time.” Whether it is the moment the patient enters the preoperative area, the start of anesthesia, or the first incision, it’s crucial that everyone is on the same page. You should also communicate the importance of starting on time, from a cost and efficiency perspective, in a positive way. This communication helps to make sure your staff can appreciate on-time starts as an aspect of providing the best service.
Many practices hold weekly team meetings, or daily huddles, as a way of keeping on top of scheduling. Documenting and communicating issues via your surgery scheduling platform also helps your team problem-solve and preempt potential problems to keep the schedule flowing.
By using a robust surgery scheduling software solution for communication, you can make sure the right people have the right information at the right time. A software solution also ensures that the messaging is consistent and accessible and that no one is left out of the loop, even if they miss a meeting. By leveraging software to close the gaps in communication, there is less burden on the already overwhelmed operating room staff on the day of surgery.
2. Analyze and utilize block time effectively
Block scheduling aims to help surgeons make the most of surgery time. But blocks must be used effectively. Surgeons need to cover as many cases as possible within their blocks, without compromising on quality or patient safety. Inaccurate estimates of procedure timings can cause delays in subsequent surgeries. A surgeon trying to squeeze as many procedures into a block as possible may fail to account for lead-in times and other processes, such as patient positioning, clean-up, and room turnover. Not factoring these processes in can lead to chronic schedule drift.
It’s also important to analyze block time use to ensure procedures are grouped or sequenced in the most effective way. For example, by scheduling predictable, complication-free procedures early in the block, schedulers can minimize the impact of later delays on overall surgery times.
Schedulers can use surgery scheduling software to ensure patients, surgeons, and staff are aware of—and prepared for—the start time. Look for software that can facilitate efficient block scheduling and pooling, for example, by color-coding cases at risk of delay, allowing schedulers to modify block allocation for greater block utilization. A good surgery scheduling software will recognize block time at high risk of going under-utilized and proactively flag cases that could fill in the unclaimed time. Modern solutions use business intelligence functionality to allow management to examine OR utilization and trends.
3. Improve time management
Poor physician punctuality can also be a cause of delays and revenue loss. One innovative approach implemented by Northwestern Medicine Lake Forest Hospital, borrowed NASA’s “T-minus” countdown as part of building urgency for on-time starts. Combined with streamlined processes, the service raised its on-time percentage from 37% to 77%.
However, there are easier ways to make improvements. Using an electronic calendar gives all stakeholders access to the up-to-date schedule, and automatically notifies all parties of updates or changes in real time. An e-calendar can also give surgeons the option to share blocks. This helps teams maximize block time and reduce delays to start times.
Not all late starts stem from staff inefficiencies. Patients can arrive late. They may be unprepared for the surgery. They may have questions or uncertainties. Automated notifications and AI-enabled Virtual Patient Guides allow patients to get questions answered efficiently while being kept up-to-speed about the timing of their procedure. Having this insight can help reduce lateness or no-shows. Conversely, when cases are completed efficiently, being able to call patients in sooner and inform the perioperative teams is also key to ensuring no interruptions in the surgical schedule. It can be very frustrating for an efficient team to have to sit idle because the preoperative team and patient were expecting a later start. Look for a software tool that can help identify and analyze factors impacting individual cases and patients.
4. Automate your data management
With up to 150 data points needed to properly schedule a single surgery, staying on top of the space, equipment, and staffing requirements for every case is a challenging task (not to mention doing so while avoiding potential conflicts and delays). If your hospital or ASC relies on paper-based or manual data-entry systems for scheduling, errors are bound to happen. Paper posting forms are time-consuming and make it harder for surgical staff surgeons to access and share key patient and procedure information.
A good surgery scheduling software platform should incorporate a digital operating room scheduling board, which allows the scheduler to update calendar changes that are visible in real time from any location. This helps to increase surgical throughput and flag cases at high risk of delay. It also produces reports of scheduler, surgeon, and service line performance.
5. Be proactive about communicating
Being prepared in advance is key to on-time start. This means ensuring all the necessary information and equipment are present and correct. A study of over 15,000 delayed cases found that the two top reasons for case delays were:
- The OR wasn’t ready for patients;
- Patient documentation was incomplete.
Missing preoperative assessments can mean the patient is not ready for surgery. Meanwhile, inaccurate or out-of-date Doctor Preference Cards (DPCs) can result in the right surgical instruments not being available or not sterile. Ensuring accuracy is more of a challenge if staff is relying on paper or locally held digital copies.
Surgical scheduling software with integrated DPC management gives surgical teams a centralized tool for ensuring all the necessary forms and the right supplies, instruments, equipment, and medications are ready for each procedure. Using AI-powered, HIPAA-compliant repository allows schedulers, pre-op staff, and surgeons to easily access the most up-to-date preferences and be ready for an on-time start.
Begin improving your on-time starts
CaseCTRL is a comprehensive, integrated software solution that makes surgery scheduling and planning more efficient. Using AI-empowered tools such as Case Builder, Intelligent Repository, Surgical Calendar, and Risk Analyzer with automatic notifications, our software can keep your team on track and drive more surgery in an automated fashion. See how CaseCTRL’s solutions can help you facilitate process change by scheduling a demo.