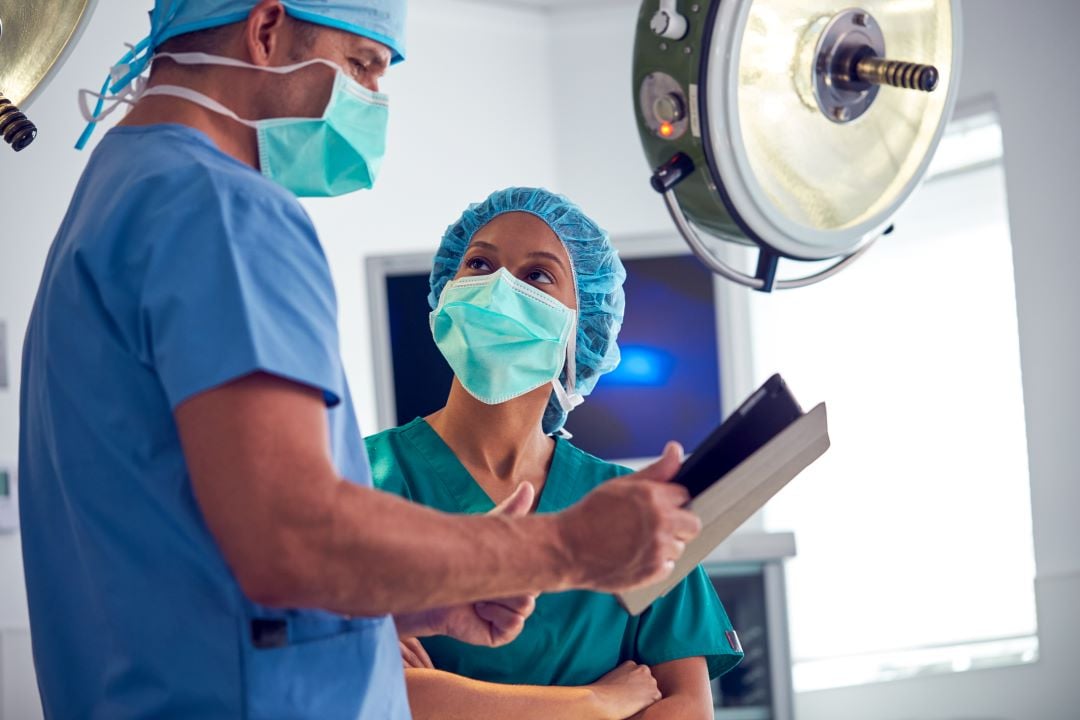
Could you be leaving $500k a year on the table just because of antiquated surgical scheduling processes that are siloed, laborious, and error-prone?
The paper-based workflows for coordinating surgeries that occur in the ambulatory setting well before most cases are entered into the hospital or ambulatory surgery centers (ASCs) EMR are highly inefficient. Without transparency earlier in the scheduling process, resources can't be shared efficiently. When these processes aren't completely trackable and measurable, you may not know where things are falling through the cracks and how you can plug the leaky bucket.
How Do Hospitals Schedule the Use of Operating Theatres (and why it's costing you)
The daily scheduling of an operating theatre is a consistent act of juggling various criteria and competing objectives. Due to the high cost of running an OR, schedulers are under tremendous pressure to maximize the use of the facilities while balancing the quality of patient care.
Inefficient scheduling (which can be caused by a breakdown in communications between surgeons and schedulers on surgical plans, case times, and other requirements) can lead to costly idle time between cases, significant overtime costs, and increased patient anxiety because of delays or rescheduling of surgery.
From surgeons estimating case time for each surgery to schedulers selecting the correct procedures, organizing all the resources, and communicating the schedule back to the surgeons accurately, many things can go wrong along the manual process.
With as many as 150 data points in one surgery, it's a challenge to orchestrate the multiple parties involved, manage staff requirements, as well as track potential conflicts and equipment needs so that you can ensure that the timeline is met. Moreover, without transparency earlier in the scheduling process, it is very hard for schedulers and groups to pool and cooperatively optimize unused operating room time, often until it’s too late.
Reliance on manual estimation and a handful of independent schedulers reduces the efficiency and accuracy of these processes. Not to mention, it's cumbersome to manually update everyone on schedule changes, yet failing to get all the personnel, tools, and supplies lined up can create a negative ripple-effect on treatment outcomes, while also leading to costly delays, cancellations, and diminished patient satisfaction.
Overcome OR Scheduling Challenges with Operating Theatre Scheduling Software
Surgeons need a more efficient and reliable way to communicate their complex surgical plans, timelines, and resource needs to schedulers so that they can effectively manage the many interlocking components. Here's why the use of operating theatre scheduling software is on the rise and how it can benefit your practice:
- Clear communication between surgeon and scheduler helps eliminate misunderstanding and ensures that the right personnel, supplies, and resources are set up correctly.
- A cloud-based platform allows everyone involved to get real-time updates to minimize errors and delays caused by schedule changes.
- Algorithms analyze similar surgeries and provide accurate case time estimation to help maximize resource usage without impacting patient experience.
- Effective coordination among the various specialists involved helps facilitate cross-disciplinary collaboration to improve treatment outcomes.
- The ability to better manage canceled surgeries allows you to prioritize and organize action items so that you can follow up and reschedule cases efficiently.
- Increase visibility into your scheduling workflows enables you to stay in control and diagnose issues in the pipeline quickly.
- Better visibility earlier in the scheduling process, across the practice, fosters sharing of under-utilized operating room resources.
- Better planning and resource allocation reduce the costly problem of having to line up excess capacity to accommodate unpredictable circumstances.
How to Choose the Right Operating Theatre Scheduling Software
Here are some important features you should look for when selecting surgical scheduling software for your practice:
Case Construction
This feature allows you to easily build customized cases and share it with the scheduler digitally so that you can be sure that every step, resource need, and personnel are accounted for. By eliminating cumbersome paper-based processes, you can also avoid errors and delays caused by lost or illegible case posting sheets.
Knowledge Repository
A HIPAA-compliant knowledge repository records all your preferences so that you don't have to rely on the availability of one or two schedulers. You have the flexibility to work with multiple schedulers, ensuring you don't risk falling behind on cases. This can eliminate lost time and money while making sure that your patients get their surgeries scheduled in a timely manner for the best outcomes. It also eliminates team dependency on the surgeon because they have a resource to consult when questions arise about the surgical treatment plan about a particular patient.
Automatic Notifications
Real-time, automated notifications keep everyone involved in the loop as soon as an adjustment is made to a case to promote a successful cross-disciplinary collaboration. You can coordinate the activities of patients, staff, assistants, vendors, anesthesia, the hospital, insurance provider, and more so that you have all the right resources lined up for each and every surgery.
Patient Communication
Timely and comprehensive patient communication helps ensure a successful procedure. An operating theatre scheduling software allows you to communicate with patients and send them relevant information. You can use an integrated AI chatbot to answer common questions so patients can get the reassurance they need without pulling you or your staff away from important tasks.
Integrated Dashboard
An easy-to-use integrated dashboard enables you to track pending, scheduled, completed, held, and canceled surgical cases all in one place. This can improve operational cost-efficiency and give you the visibility to properly manage your pipeline so that you can stop leaving money on the table simply because something gets lost in the shuffle. Patients often have to delay surgeries for many personal reasons such as financial constraints, insurance changes, or lack of support. Mechanisms to maintain a dialogue with these patients are key to demonstrating compassion and ensuring these patients return to the practice when circumstances are more favorable.
Risk Assessment
Predictive analytics incorporating recognized anesthesia, cardiology, and surgery specific guidelines for perioperative care can analyze patient- and case-specific risk factors to help you proactively avoid pitfalls that could impact patient satisfaction and treatment outcomes. For example, you can identify patients who should receive pre-operative clearance and can benefit from inpatient admission, as well as cases that are at high risk for readmission and complications to inform better decision-making. With the migration to value-based care and bundle payments, anticipating such pitfalls are critical to the bottom line.
Resource Allocation
An intelligent resource allocation tool integrates requirements from a hospital/ASC, surgeon, patient, and other specialists to optimize case scheduling sequences and block time based on real-time shifts in scheduling and resource availability. You can maximize the use of available resources and minimize the cost of over-capacity without compromising the patient experience.
Surgery Scheduling Software Built by Surgeons for Surgeons
How do we know that all these features will work for your practice? Because we're surgeons too.
That's why we have built CaseCTRL from the ground up based on our from-the-trenches experience to help you optimize your OR schedule, create complex cases with ease, allocate your resources intelligently, and manage your communication effortlessly.
Learn more about CaseCTRL and get in touch to see how we can help you manage your surgical scheduling cost-efficiently here.